Come see HTS at the Leading Age Indiana Spring Conference on Monday, May 6th!
Indianapolis Convention Center, Indianapolis, IN
Booth 203 & 205
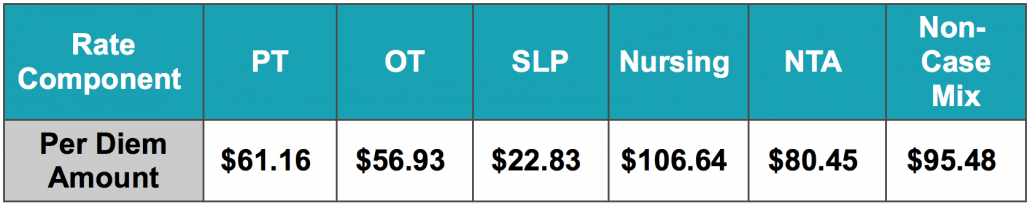
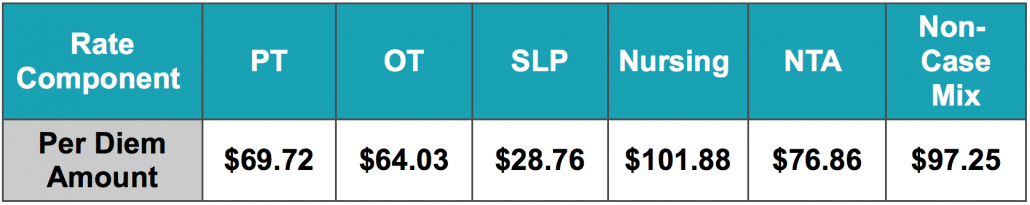
To go along with our Power Through PDPM education, be sure to pick up your very own Apple or Android LED Phone Charger!
And our very own Amanda Green, Executive Director of Marketing & Strategic Development, will be presenting…

Collaborating on Care Transitions
Monday, May 6 | 4:00 – 5:00 PM
What if…all of the companies interacting with your discharging resident worked together instead of operating by their own agenda? We’ve turned the care transition process on its head through strategic collaboration focused on communication, best practice and person-centered discharge practice.
Faculty: Amanda Green (Healthcare Therapy Services, Inc.), Mark Prifogle (GrandView Pharmacy), and Panelists (The Towne House Retirement Community).